The thymus is a small organ at the top of the chest, in which T cells develop. These developing T cells are exposed to practically all of the possible proteins that they may encounter in the body. This exposure ensures that T cells recognizing the body’s own antigens are deleted, as they constitute a potential threat and may cause autoimmunity, whereas functionally competent T cells that do not bind any of the self-proteins survive. Traditionally, most attention has been paid to the thymic epithelial cells, which are primarily responsible for this process. However, the thymus could not form without a network of fibroblast cells to form this critical support structure. Until recently those fibroblasts were relegated to supporting players within the thymus.
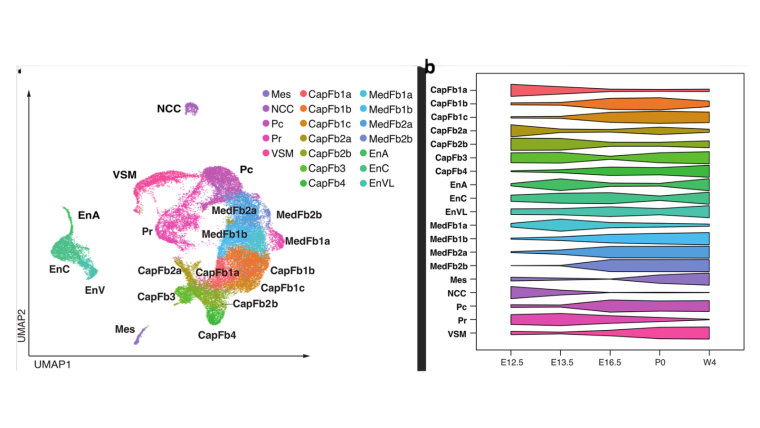
The new study from the Holländer’s lab led by Adam Handel and Stanley Cheuk uses single cell sequencing approaches to focus on those frequently overlooked fibroblasts cell-by-cell across mouse and human development. Far from being dull structural cells, fibroblasts in the thymus are now appreciated to have a wide variety of features that allow them to be classified into separate subtypes (Fig. 1a). Moreover, the proportion of these fibroblast subtypes within the thymus changes dramatically over the ageing process (Fig. 1b). This suggests that dynamic changes in fibroblast subtypes are important in shaping the thymus as it develops.
In tandem, the authors noticed that a group of cells expressing genes characteristic of neural crest cells were found in both mouse and human thymus samples. These were previously shown to be vital in the development of blood vessels within the thymus. Handel and colleagues used bioinformatic tools to show that substances produced by the neural crest cells and cells around blood vessels were important in driving the ageing process. Additionally, by using a novel single cell method of relating gene expression to the accessibility of DNA to gene regulatory factors, this study was able to identify key regions determining the control of master regulators of neural crest cell identity through testing the extent to which accessibility of DNA near the SOX10 gene could predict its expression.
Changes in fibroblast subtypes were also seen to be important in the DiGeorge syndrome, one of the commonest genetic conditions affecting the thymus. The authors showed that mice which were engineered to have genetic changes characteristic of the DiGeorge syndrome had lost many cells from within specific fibroblast subtypes, particularly those that make up blood vessels. DiGeorge syndrome has previously been shown to cause problems in neural crest development, so it is likely that the changes in neural crest signalling over age identified in the paper may also impact on thymic development in this genetic disorder.
Overall, Handel, Cheuk and colleagues showed that structural cells in the thymus should never be considered boring.
View full research article via the Science Advances website.